Ultrasound-Guided External Oblique Intercostal Plane Block
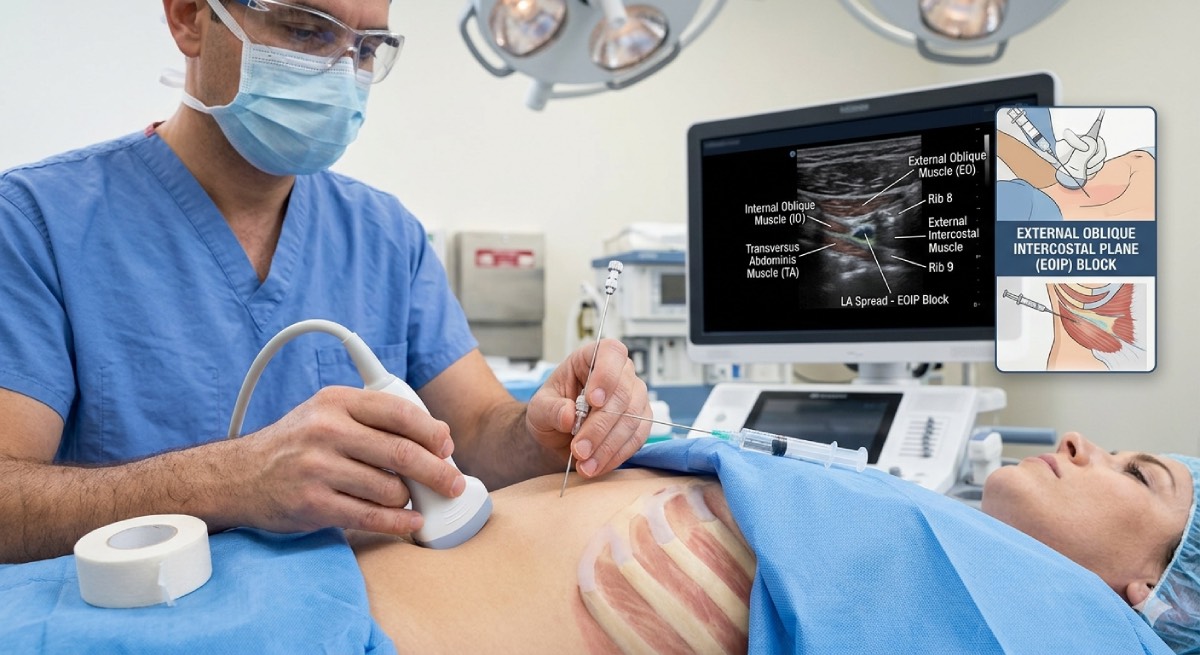
The ultrasound-guided external oblique intercostal plane block is a regional anesthesia technique used to provide effective analgesia for upper abdominal and thoracic wall surgeries. Its use has gained attention in both acute postoperative pain control and multimodal analgesia strategies, particularly due to the high accuracy offered by ultrasound guidance.
The external oblique intercostal plane block targets the intercostal nerves as they travel in the fascial plane between the external oblique muscle and the intercostal muscles. These nerves arise from the thoracic spinal nerves and supply sensation to the upper abdominal wall. By depositing local anesthetic in this specific plane, the block effectively interrupts pain signals from surgical sites in the upper abdomen and lower chest.
The procedure is carried out under ultrasound guidance to ensure accuracy and safety. The patient is typically positioned supine, and a high-frequency linear ultrasound probe is placed along the anterior axillary line over the lower ribs. The external oblique muscle is identified as the most superficial muscle layer. A needle is then advanced in-plane under real-time visualization into the fascial plane between the external oblique and intercostal muscles. Once the correct position is confirmed, local anesthetic is injected, spreading along the plane to cover multiple intercostal nerves 1,2.
A main advantage of this block is its safety profile. Because the injection is made in a superficial plane, the risk of complications such as pneumothorax or vascular injury is relatively low compared to deeper blocks. In addition, ultrasound guidance improves precision and reduces the likelihood of incorrect placement. The technique is also relatively easy to learn for clinicians experienced in ultrasound-guided procedures.
Ultrasound-guided external oblique intercostal plane block is particularly useful for surgeries involving the upper abdomen, such as laparoscopic cholecystectomy, liver surgery, and certain hernia repairs, but can also be used in rib fractures and thoracic trauma for pain control, among other applications. By providing localized analgesia, it reduces the need for systemic opioids and enhances patient recovery 3–5.
Despite its benefits, the ultrasound-guided external oblique intercostal plane block has a number of limitations. The duration of analgesia is dependent on the type and volume of local anesthetic used, which may require repeat dosing or catheter placement for prolonged pain control. There also remains a certain degree of variability in the spread of the anesthetic, which can affect the consistency of analgesia. On top of that, as a relatively new technique, there is limited large-scale clinical data compared to more established regional blocks.
Recent studies aim to assess the relative effectiveness of this block in various surgical settings and compare it with other regional anesthesia techniques. A case series published by Liotiri et al. reported that it provided sufficient analgesia as the primary regional anesthesia technique following open pancreatoduodenectomy, compared to their previous protocol of using thoracic epidural anesthesia 6. A meta-analysis of existing literature found that it provides effective analgesia compared to fascial plane block, but the dearth of high-quality evidence necessitates further research7.
The ultrasound-guided external oblique intercostal plane block is a promising addition to regional anesthesia techniques. With its targeted approach, favorable safety profile, and capacity to reduce opioid use, it represents an important advancement in modern pain management. Continued research and clinical experience will further define its place in surgical and trauma care.
References
1. Mistry, T., Sharma, S. K. & Sonawane, K. B. External oblique intercostal plane block: Anatomical landmark-guided technique! Indian J Anaesth 68, 504–505 (2024). DOI: 10.7759/cureus.61617
2. White, L. & Ji, A. External oblique intercostal plane block for upper abdominal surgery: use in obese patients. British Journal of Anaesthesia 128, e295–e297 (2022). DOI: 10.1016/j.bja.2022.02.011
3. Thakore, S., Mistry, T., Nair, A. S. & Kaasat, A. External oblique intercostal plane block: A scoping review of anatomy, techniques, and clinical applications. Indian J Anaesth 70, 157–176 (2026). DOI: 10.4103/ija.ija_1019_25
4. Zhang, J. External Oblique Intercostal Plane Block for Postoperative Analgesia After Major Upper Abdominal Surgery: A Randomized Controlled Trial. https://clinicaltrials.gov/study/NCT07331441 (2025).
5. Sinha, C. & Nambiar, S. OP33 Analgesic efficacy of ultrasound guided external oblique intercostal plane block in pediatric patients undergoing upper abdominal surgeries: a randomized clinical trial. Reg Anesth Pain Med 50, A22–A22 (2025). DOI: 10.4103/ija.ija_484_25
\6. Liotiri, D., Diamantis, A. & Zacharoulis, D. External oblique intercostal block with continuous catheter technique: use in enhanced recovery after pancreatic surgery. British Journal of Anaesthesia 134, 1187–1189 (2025). DOI: 10.1016/j.bja.2024.12.016
7. Saran, A. et al. External oblique intercostal plane block for postoperative analgesia: A systematic review and meta-analysis of randomised controlled trials. Indian J Anaesth 70, 27–40 (2026). DOI: 10.4103/ija.ija_1074_25
