Administration of Sedation by Physician Assistants
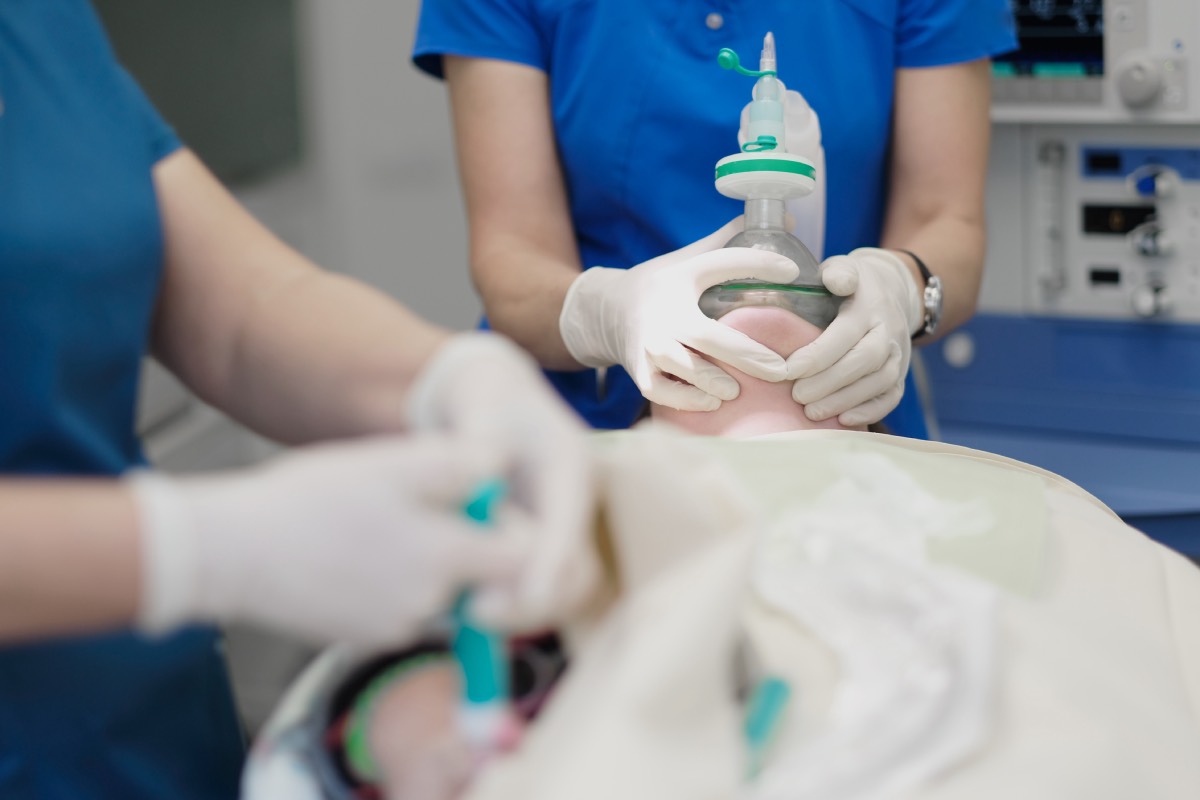
Sedation is commonly used in medical procedures to reduce anxiety, discomfort, and pain while allowing patients to remain responsive or lightly asleep. Physician assistants play an important role in delivering healthcare in many settings, and in some cases, they may be involved in administering or managing sedation. This practice is guided by strict training requirements, legal regulations, and institutional policies to ensure patient safety.
Physician assistants are licensed medical professionals who work under the supervision of physicians. They are trained to perform physical exams, diagnose conditions, order tests, assist in surgeries, and provide treatment. Their responsibilities vary depending on state laws, hospital policies, and the supervising physician’s scope of practice. Since sedation involves medications that can affect breathing, heart rate, and consciousness, it is considered a higher-risk medical task that requires advanced training and careful monitoring 1,2.
Sedation ranges from minimal sedation, where patients are relaxed but fully awake, to deep sedation, where patients are difficult to arouse and may need help maintaining their airway. Moderate sedation allows patients to respond to verbal commands while feeling calm and comfortable. The deeper the level of sedation, the higher the risk of complications such as breathing problems or low blood pressure. Therefore, the level of sedation determines who may administer it and what monitoring is required 3,4. In general, under the supervision of a physician and in accordance with state and facility regulations, physician assistants may be able to administer medications that qualify as minimal sedation. Less commonly, they may be able to administer medications for moderate sedation, also depending on regulations and privileges.
Before a physician assistant can participate in administering sedation, they must receive specific education in pharmacology, airway management, patient monitoring, and emergency response. Many healthcare institutions require additional certifications, such as Advanced Cardiac Life Support (ACLS). Supervised practice is also necessary, and ongoing education is often required to maintain these privileges 5–7.
Some states allow physician assistants to administer minimal sedation or minimal to moderate sedation under physician supervision. Hospitals and surgical centers usually have credentialing committees that review a physician assistant’s training and determine what procedures they are permitted to perform. These rules are designed to ensure that sedation is only given by providers who are fully qualified 8–10.
When sedation is administered, continuous monitoring is essential. Vital signs such as heart rate, oxygen levels, blood pressure, and breathing are closely observed. Physician assistants involved in sedation, whether in medication administration or in patient monitoring, must be able to recognize early signs of complications and respond quickly—to this end, emergency equipment and medications must be immediately available. Clear communication among the medical team is also critical, especially when procedures are being performed at the same time as sedation is being managed 11–13.
Patient safety and informed consent are central to ethical sedation practices. Patients should be informed about who will administer their sedation and what level of supervision is present; transparency helps build trust and ensures that patients understand their care. Physician assistants are expected to work within their training and to seek physician support whenever needed, especially if a patient’s condition changes 14–16.
References
1. Hilbert, J. The Vital Role of Physician Assistants in Patient Care. Shore Physicians Group https://shorephysiciansgroup.com/the-vital-role-of-physician-assistants-in-patient-care/ (2023).
2. Science, M. C. C. of M. and. Physician Assistant – Explore Healthcare Careers – Mayo Clinic College of Medicine & Science. Mayo Clinic College of Medicine and Science https://college.mayo.edu/academics/explore-health-care-careers/careers-a-z/physician-assistant/.
3. Types of Sedation. Association of Hospital Anesthesiologists https://www.foxcitiesaha.com/about-anesthesia/about-anesthesia/types-of-sedation/.
4. Statement on Continuum of Depth of Sedation: Definition of General Anesthesia and Levels of Sedation/Analgesia. https://www.asahq.org/standards-and-practice-parameters/statement-on-continuum-of-depth-of-sedation-definition-of-general-anesthesia-and-levels-of-sedation-analgesia.
5. Advanced Cardiovascular Life Support (ACLS). cpr.heart.org https://cpr.heart.org/en/cpr-courses-and-kits/healthcare-professional/acls.
6. MS, D. S. M., DMSc, PA-C. PAs and Advanced Airway Training: the Intubation Consternation. Clinical Advisor https://www.clinicaladvisor.com/home/my-practice/physician-assistant-career-resources/physician-associates-advanced-airway-techniques/ (2023).
7. Guest, B. N., Chandrakanthan, C., Bascombe, K. & Watkins, J. Pharmacology for physician associate programmes: a collaborative, flexible and responsive approach to curriculum design. Future Healthc J 8, e580–e584 (2021). DOI: 10.7861/fhj.2021-0099
8. H-35.989 Physician Assistants | AMA. https://policysearch.ama-assn.org/policyfinder/detail/H-35.989?uri=%2FAMADoc%2FHOD.xml-0-2996.xml.
9. Working with physician assistants: Regulation, delegation, and liability protection. CMPA https://www.cmpa-acpm.ca/en/advice-publications/browse-articles/2024/working-with-physician-assistants-regulation-delegation-and-liability-protection.
10. Physician Assistants, Legal and Ethical Use in Practice. https://www.ttlhealthlaw.com/health-law-blog/details/health-law-blog/2020/09/04/physician-assistants-legal-and-ethical-use-in-practice.
11. Standards for Basic Anesthetic Monitoring. https://www.asahq.org/standards-and-practice-parameters/standards-for-basic-anesthetic-monitoring.
12. O’Daniel, M. & Rosenstein, A. H. Professional Communication and Team Collaboration. in Patient Safety and Quality: An Evidence-Based Handbook for Nurses (ed. Hughes, R. G.) (Agency for Healthcare Research and Quality (US), Rockville (MD), 2008).
13. Sheahan, C. G. & Mathews, D. M. Monitoring and delivery of sedation. British Journal of Anaesthesia 113, ii37–ii47 (2014). DOI: 10.1093/bja/aeu378
14. The clinician-patient relationship in the era of information transparency – UpToDate. https://www.uptodate.com/contents/the-clinician-patient-relationship-in-the-era-of-information-transparency.
15. Robins, L. et al. Identifying transparency in physician communication. Patient Education and Counseling 83, 73–79 (2011). DOI: 10.1016/j.pec.2010.05.004
16. Ethical Guidelines for the PA Profession. AAPA https://www.aapa.org/career-central/practice-tools/ethical-guidelines-for-the-pa-profession/.
